Epidemics of the Past: Smallpox: 12,000 Years of Terror
Smallpox: 12,000 Years of Terror
Smallpox is one of greatest scourges in human history. This disease, which starts with a distinctive rash that progresses to pus-filled blisters and can result in disfiguration, blindness, and death, first appeared in agricultural settlements in northeastern Africa around 10,000 B.C.E. Egyptian merchants spread it from there to India.
The earliest evidence of smallpox skin lesions has been found on the faces of mummies from the eighteenth and twentieth Egyptian dynasties, and in the well-preserved mummy of Pharaoh Ramses V, who died in 1157 B.C.E. The first recorded smallpox epidemic occurred in 1350 B.C.E., during the Egyptian-Hittite War.
In 430 B.C.E., the second year of the Peloponnesian War, smallpox hit Athens and killed more than 30,000 people, reducing the population by 20 percent. Thucydides, an Athenian aristocrat, provided a terrifying account of the epidemic, describing the dead lying unburied, the temples full of corpses, and the violation of funeral rituals. Thucydides himself had the disease, but he survived and went on to write his historic account of the Peloponnesian War. In this work, he noted that those who survived the disease were later immune to it. He wrote, “the sick and the dying were tended by the pitying care of those who had recovered, because they knew the course of the disease and were themselves free from apprehensions. For no one was ever attacked a second time, or not with a fatal result.” These Athenians had become immune to the plague.
Athens was the only Greek city hit by the epidemic, but Rome and several Egyptian cities were affected. Smallpox then traveled along the trade routes from Carthage.
Potent Fact
Rhazes was a Persian doctor who worked in the main hospital of Baghdad. He ranks with Hippocrates and Galen as one of the founders of clinical medicine and is widely regarded as the greatest physician of Islam and the Medieval Ages. His writings on medicine influenced physicians well through the Renaissance and into the seventeenth century. And his work on smallpox and measles was one of the first scientific treatments of infectious diseases.
In 910, Rhazes (Abu Bakr Muhammad Bin Zakariya Ar-Razi, 864-930 C.E.) provided the first medical description of smallpox, documenting that the illness was transmitted from person to person. His explanation of why survivors of smallpox do not develop the disease a second time is the first theory of acquired immunity.
The patterns of disease transmission often paralleled peoples' travel and migration routes. Disease in Asia and Africa spread to Europe during the Middle Ages. Smallpox was brought to the Americas with the arrival of Spanish colonists in the fifteenth and sixteenth centuries, and it is widely acknowledged that smallpox infection killed more Aztec and Inca people than the Spanish Conquistadors, helping to destroy those empires.
Smallpox continued to ravage Europe, Asia, and Africa for centuries. In Europe, near the end of the eighteenth century, the disease accounted for nearly 400,000 deaths each year, including five kings. Of those surviving, one-third were blinded. The worldwide death toll was staggering and continued well into the twentieth century, where mortality has been estimated at 300 to 500 million. This number vastly exceeds the combined total of deaths in all world wars.
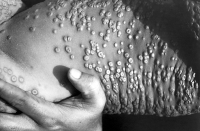
This person, photographed in Bangladesh, has smallpox lesions on skin of his midsection. (Courtesy CDC/James Hicks)
In the United States, more than 100,000 cases of smallpox were recorded in 1921. Strong declines occurred after that because of the widespread use of preventive vaccines. By 1939, fewer than 50 Americans per year died of smallpox.
Variolation: The Earliest Smallpox “Vaccines”
The idea of intentionally inoculating healthy people to protect them against smallpox dates back to China in the sixth century. Chinese physicians ground dried scabs from smallpox victims along with musk and applied the mixture to the noses of healthy people.
In India, healthy people “protected” themselves by sleeping next to smallpox victims or wearing infected peoples' shirts. In Africa and the Near East, matter taken from the smallpox pustules—raised lesions on the skin the contain pus—of mild cases was inoculated through a scratch in an arm or vein. The goal was to cause a mild infection of smallpox and stimulate an immune response that would give the person immunity from the natural infection. This process was called variolation. Unfortunately, the amount of virus used would vary and some would contract smallpox from the inoculation and die. Nonetheless, this preventive approach became popular in China and South East Asia. Knowledge of the treatment spread to India, where European traders first saw it.
Disease Diction
Variolation is the inoculation of matter taken from the smallpox pustules of mild cases through a scratch in an arm or vein. Used by people in the past, the goal was to cause a mild infection of smallpox and stimulate an immune response that would give the person immunity from the natural infection.
An Englishwoman, Lady Mary Wortly Montagu, was responsible for introducing variolation to England. In 1717, while accompanying her husband, the British ambassador to Turkey, in Constantinople she came across the ancient Turk practice of inoculating children with smallpox matter.
Initially horrified at this seemingly savage practice, she learned that a child was protected from the ravages of smallpox through this process. She then had her six-year-old son inoculated while in Turkey, and in 1721, in the presence of Royal Society Members, she had her daughter inoculated. This led to adoption of variolation, mainly by the aristocracy in England and Central Europe. Before long, variolation to prevent smallpox was widespread. During America's War of Independence, George Washington had his army treated in this way. Napoleon did the same with his army before they invaded Egypt.
Edward Jenner: Vaccine Pioneer
During his training as a physician, Edward Jenner learned from nearby milkmaids that after they contracted cowpox they never got smallpox. Cowpox is a far milder disease than smallpox, yet the diseases are quite similar. In 1796, Jenner decided to test the theory that infectious material from a person with a milder similar disease could protect against a more severe disease.
He put some pus from a cowpox pustule on small cuts made on the arm of James Phipps, an eight-year-old boy. Eight days later, Phipps developed cowpox blisters on the scratches. Eight weeks later, Jenner exposed the child to smallpox. The boy had no reaction at all, not even a mild case of smallpox. The cowpox had made him immune to smallpox. Jenner developed the first vaccine, using cow serum containing the cowpox virus. Jenner tried this new treatment on eight more children, including his own son, with the same positive result.
Potent Fact
The word vaccination is derived from the Latin word for cow, vacca.
After a period of slow acceptance, Jenner's vaccine approach was widely adopted. Vaccination using Jenner's method was key in decreasing the number of smallpox deaths, and it paved the way for global eradication of the disease.
The World Takes Action
In 1959, The World Health Assembly decided to organize mass immunization campaigns against smallpox. The World Health Organization (WHO) announced the global smallpox eradication program in 1967. At that time there were still an estimated 10 to 15 million cases of smallpox a year resulting in two million deaths, millions disfigured, and another 100,000 blinded. Ten years later, after dispersal of 465 million doses of vaccine in 27 countries, the last reported naturally occurring case appeared in Somalia. On October 22, 1977, a 23-year-old male, Ali Maow Maalin, developed smallpox and survived.
Potent Fact
Amazingly, eradication of smallpox, one of the world's most deadly scourges, cost approximately $100 million. Even in today's dollars, this was a bargain.
The global campaign against smallpox ended in 1979 just two years after Maalin's case. Two additional cases of smallpox occurred in Birmingham, England, in 1978, after the virus escaped from a laboratory. There has not been a case reported in more than 25 years.
Variola: The Cause of Smallpox
Smallpox is caused by a virus and can result in one of two forms of the disease, called variola major and variola minor. Variola major kills 20 to 40 percent of unvaccinated people who get it and can lead to blindness. Variola minor, a far less lethal form of the disease, results in death only on rare occasions.
Disease Diction
A sixth-century Swiss bishop named the cause of smallpox variola, from the Latin varius, meaning “pimple” or “spot.” In the tenth century, the term poc or pocca was used to describe the scars left behind, which resembled “pouches.” When syphilis became epidemic in the fifteenth century, the term smallpox was adapted to distinguish between the diseases.
The disease is transmitted primarily by direct contact with droplets from saliva and other body fluids that travel through the air, such as through a sneeze. It may also be spread if an uninfected person handles clothing worn by someone with the disease.
Signs and Symptoms of Smallpox
The incubation period for smallpox is 8 to 17 days, with people usually getting sick 10 to 12 days after infection. Symptoms start with malaise, fever, rigors, vomiting, headache, and backache. The trademark smallpox rash appears after two to four days, first on the face and arms and later on the legs, quickly progressing to red spots, called papules and eventually to large blisters, called pustular vesicles, which are more abundant on the arms and face. Although full-blown smallpox is unique and easy to identify, earlier stages of the rash could be mistaken for chickenpox. When fatal, death occurs within the first or second week of the illness.
There is no effective treatment for smallpox. There are antiviral drugs that might work, but they have not been tested due to restrictions on smallpox research.
Smallpox Vaccine
The smallpox vaccine currently licensed in the United States is made with a virus called vaccinia, which is related to smallpox. It does not contain the actual smallpox (variola) virus. Vaccinia causes the body to produce antibodies that protect against smallpox and several other related viruses.
When a person is vaccinated, the usual response is the development of a red spot atthe vaccination site two to five days after the shot. The red spot becomes pustular, and reaches its maximum size in 8 to 10 days. The pustule dries and forms a scab, which separates 14 to 21 days after vaccination, leaving a scar. Sometimes there is also swelling and tenderness of lymph nodes. A fever is common after vaccine. Fatal complications are rare, with less than one death per million vaccinations.
The CDC is the only source of smallpox vaccine and will provide it to protect laboratory and other health-care personnel at risk for exposure. A reformulated vaccine is now under development.
Smallpox: An Agent of Bioterrorism?
Potent Fact
There were approximately 15 million doses of 20-year-old vaccine available following the September 11, 2001, terror attacks. However, once bioterrorism in the form of anthrax became a real threat, the United States government urgently ordered another 150 million doses of smallpox vaccine to be made available within short order as a precaution.
Several years ago, Ken Alibek, a former deputy director of the Soviet Union's civilian bioweapons program, indicated that the former Soviet government had developed a program to produce smallpox virus in large quantities and adapt it for use in bombs and intercontinental ballistic missiles.
If a smallpox vaccine exists, smallpox bioterrorism shouldn't be a problem, right? Wrong. The vaccine program in the United States was so successful that routine vaccination was discontinued in 1972. Nearly 50 percent of the population has never been vaccinated and, of the vaccinated individuals, the vaccine is of questionable value since it requires boosting every 10 years. For the first time in nearly a century, the United States population is at significant risk for smallpox.
By international agreement, the main stores of smallpox virus from the Cold War superpowers are kept securely at the CDC's headquarters in Atlanta and at a similar institute in Moscow.

Excerpted from The Complete Idiot's Guide to Dangerous Diseases and Epidemics © 2002 by David Perlin, Ph.D., and Ann Cohen. All rights reserved including the right of reproduction in whole or in part in any form. Used by arrangement with Alpha Books, a member of Penguin Group (USA) Inc.
